Quick Links
Health Care Cost Containment
Section I: Introduction
The Commonwealth is a national leader in ensuring access to quality, affordable health insurance. More than 98% of our residents have coverage, the highest rate of coverage in the nation – with nearly all children (99.8%) and seniors (99.6%) insured.

Source: Massachusetts Division of Health Care Finance and Policy. Key Indicators Report. November, 2010.
Racial and ethnics disparities in coverage have been significantly reduced. Since the enactment of health care reform, an even higher percentage of Massachusetts employers are offering health insurance to their employees, bucking a national trend.
Evidence of the impact of health care reform in Massachusetts is clear. Thousands who formerly relied on receiving care in over-burdened emergency rooms now have access to primary care through their own doctors. More than 90% of adults in Massachusetts report having a regular source of care. Since reform more adults are making a visit for preventive care, and 63% of men have had colonoscopies.
Health care reform benefits not just our residents but also our economy. Healthier people mean a more productive workforce for the Commonwealth. Likewise, investing in health care strengthens our world-renowned medical sector –where interventions ranging from improved routine care for diabetics to life-saving interventions for rare conditions save lives - and as an engine for job creation; and a magnet for research dollars and human talent. The Administration’s separate, ground-breaking investment in life sciences creates enormous potential synergies with our commitment to health care reform, together ensuring Massachusetts’ status as the world leader in health care.
.
The success of the Massachusetts model is also reflected in the enactment of national health care reform (the Patient Protection and Affordable Care Act). National health reform is based significantly on our approach in the Commonwealth, requiring all states to set up Exchanges modeled on the Massachusetts Health Connector, requiring those who can afford coverage to maintain it, reforming insurance laws to open the doors to coverage for all consumers, and broadening access to subsidized health insurance for those who need it. With our leadership in coverage expansion, we are poised to implement national reform in Massachusetts successfully and broaden opportunities for affordable coverage for our residents.
The Patrick-Murray Administration is deeply committed to the successful implementation of health care reform, partnering with the Legislature to provide policy leadership on key implementation decisions and the funding needed to offer affordable coverage to those in need. Much of the success of health care reform is due to a strong community effort, relying on partnerships with providers, insurers, consumers and businesses to ensure that health coverage is accessible, understandable, and comprehensive. Throughout the most profound economic downturn of our time, these stakeholders worked with the Administration and Legislature to maintain coverage. As unemployment rose nationally and here in Massachusetts, access to affordable coverage through our health reform initiatives kept the Commonwealth’s residents healthy.
The Administration has carefully managed the finances of health care reform. Independent, non-partisan analysis underscores that the incremental state costs of health care reform have been moderate and in line with original expectations. Recent enrollment growth in state-subsidized coverage is a natural consequence of an economic downturn and a sign of strength of the Massachusetts model, protecting coverage for residents who have lost their jobs. Private health insurance (largely through employment) remains the dominant form of coverage in the Commonwealth.
However, while the incremental costs of health care reform have been moderate, the total costs of state-subsidized coverage create a difficult challenge for the Commonwealth. These costs – a function of our eligibility standards and enrollment, the frequency with which care is sought, and how and where care is provided – are occupying an ever-increasing share of the state budget. Spending in state subsidized health care programs have grown by double digits since fiscal year 2008 while other programs like Local Aid, higher education, public safety, environmental protection services, and economic development have all been reduced. Health care spending for our subsidized coverage programs consumes more than 35% of the state budget. Based on long term forecasts conducted by the Executive Office for Administration and Finance, were health care costs were able to continue to grow at these historic rates it would consume approximately 50% of state spending by 2020. Health care spending has been crowding out key public investments that, among other things, likewise significantly impact the health and welfare of our citizens and the historic trends are unsustainable. While all states are struggling with the growth of health care spending, the higher cost of care in Massachusetts means that employers, families and municipalities are also wrestling with the ongoing challenge of choosing between health care and spending on job creation and other family and public needs.
These are not insurmountable challenges. There are opportunities to control health care costs by promoting care delivery in lower-cost, high-quality settings, improving the coordination and management of care, placing a greater focus on prevention, and adopting innovative payment models that reward high-value care instead of high-volume care. With the scale of the health insurance coverage it purchases, the state is well-positioned to capitalize on these opportunities and drive positive innovation in our health care insurance and delivery systems, containing costs while maintaining coverage and improving quality of care. The state also has opportunities to achieve greater efficiencies and continuity of coverage within state-subsidized programs by aligning coverage standards and coordinating on procurements. Taking advantage of these opportunities is particularly imperative for fiscal year 2012, where the elimination of enhanced federal Medicaid matching funds as a budget-balancing tool renders the need for immediate action to achieve health care cost savings imperative.
Governor Patrick’s and Lieutenant Governor Murray’s fiscal year 2012 budget seizes the moment to achieve ground-breaking progress in health care cost containment – with a vision for maintaining the Commonwealth’s historic coverage gains and high-quality care while making health care spending more affordable for the state and taxpayers. For each of the state’s health care programs -- MassHealth, Commonwealth Care, the Group Insurance Commission and the Medical Security Program – the budget proposes bold changes emphasizing the power of competition and innovative contracting to promote continued access to coverage and high-quality care while achieving significant cost savings. The Administration’s goal is to leverage the state’s immense purchasing power to be a force for rewarding models that provide cost-effective, high-quality coverage and care to those who rely on state health insurance and better coordinate government’s health care purchasing decisions. It would maintain eligibility for all state-subsidized health insurance programs – under the most generous eligibility standards in the nation (see below).
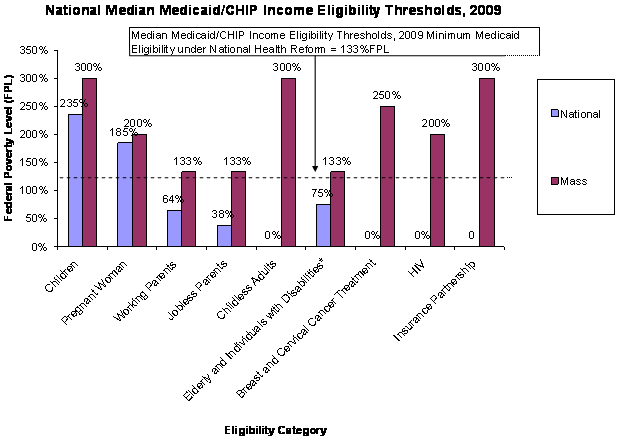
Note: Medicaid income eligibility for most elderly and individuals with disabilities is based on the income threshold of Supplemental Security Income (SSI).SOURCE: Based on a national survey conducted by the Center on Budget and Policy Priorities for Kaiser Commission on Medicaid and the Uninsured, 2009.
* Senior and disabled individuals can be up to any income if they meet a certain buy-in criteria
Separately, the Administration is planning on filing comprehensive payment reform legislation in the coming weeks that will, across the health care delivery system, promote movement away from “fee-for-service” payments to providers towards “global payments” and other models that better reward evidence-driven, coordinated, preventive care. In combination with the Administration’s budget initiatives, this legislation will place Massachusetts squarely in the forefront of national efforts to contain health care costs while ensuring high-quality coverage and care.
Section II: Health Coverage
MassHealth
The Massachusetts Medicaid program (MassHealth) provides comprehensive health insurance to approximately 1.29 million low-income Massachusetts children, adults, seniors and people with disabilities. The Administration’s fiscal year 2012 budget includes $10.34 billion for MassHealth, essentially level funding from the fiscal year 2011 estimated spending level of $10.24 billion. Due to tremendous fiscal pressures in fiscal year 2012 stemming principally from the loss of more than $1.2 billion in enhanced federal matching funds, the Administration established aggressive spending targets for all state programs, in some cases reducing funding below fiscal year 2011 levels.
Massachusetts is not the only state with a Medicaid budget that has experienced exceptional growth. Medicaid budgets across the nation have experienced unprecedented spending increases. Enrollment in Medicaid historically mirrors trends in the economy, with more individuals turning to public assistance during tougher times. Total Medicaid spending growth averaged 8.8% across all states in fiscal year 2010, and spending is expected to increase by 7.4% in fiscal year 2011. Enrollment growth averaged 8.5% nationally and is expected to decrease to 6.1% in fiscal year 2011.[1]
While Massachusetts is experiencing the same caseload and spending pressures, our projected increases in these areas are well below national benchmarks. This is likely attributable to a stronger health insurance coverage base prior to the economic downturn.

Enrollment and utilization are the greatest cost drivers in MassHealth and are sensitive to changes in economic climate. From fiscal year 2008 to fiscal year 2010, long-term unemployed adults (unemployed for 12 months or more) represented the fastest growing population in Medicaid, increasing by an average of 16.6% each year. Non-disabled adults represent the next highest category of growth, increasing by an average of 4.44%. Overall, from fiscal year 2008 through fiscal year 2011, MassHealth enrollment grew by approximately 146,000 people.
| MassHealth Average Enrollment (in Member Months) | |||||
| Fiscal year 2008 | Fiscal year 2009 | Fiscal year 2010 | Projected fiscal year 2011 | Projected fiscal year 2012 | |
| Non Disabled Children | 459,712 | 469,618 | 486,806 | 501,815 | 519,700 |
|---|---|---|---|---|---|
| Non Disabled Adults | 263,247 | 273,315 | 283,176 | 297,685 | 314,181 |
| Disabled Children | 26,501 | 26,510 | 27,371 | 29,273 | 30,424 |
| Disabled Adults | 207,559 | 210,506 | 213,952 | 223,585 | 232,326 | Long Term Unemployed Adults | 66,921 | 79,642 | 96,221 | 110,782 | 124,235 |
| Seniors | 125,483 | 125,874 | 128,380 | 132,194 | 134,658 |
| Total | 1,149,423 | 1,185,465 | 1,235,907 | 1,295,335 | 1,355,523 |
| % change | 3.1% | 4.3% | 4.8% | 4.6% | |
Medicaid continues to be a primary source of health care for low-income children, and projected to be the largest MassHealth population group at 41% in fiscal year 2012. The senior and disabled populations account for almost 30% of enrollment and more than 60% of total MassHealth spending. Programs experiencing the largest annual cost increases are those that serve seniors and the disabled.
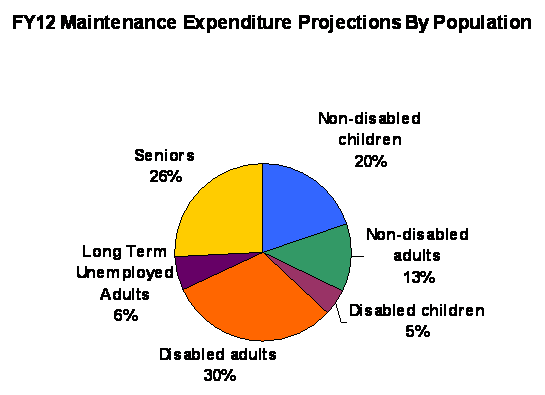
Payments to MCOs have increased annually by an average of 12.43% from fiscal year 2008 to projected trends in fiscal year 2011, primarily due to an enrollment increase of 86,400 members over four years and federal requirements to maintain actuarially sound rates. Without smart cost-saving changes to MassHealth, the Commonwealth could face an $800 million shortfall in fiscal year 2012 and the prospect of across-the-board cuts to services. Even beyond the need to achieve savings to address immediate, economy-driven fiscal challenges facing MassHealth, containing MassHealth costs is critical to the long-term sustainability of health care reform and the long-term ability of the state budget to invest in the full range of public needs. Success on this front would not only maintain our health care safety net for all who need it as well as facilitate other key public investments, but also – given the scale of MassHealth – drive positive innovation in the delivery of care throughout our health care system.
Given these short- and long-term challenges and opportunities, MassHealth will be pursuing aggressive strategies to manage its fiscal year 2012 budget. Unlike other state programs, MassHealth costs are difficult to constrain, since expenditures are driven by caseload and eligibility is primarily controlled by eligibility standards fixed by the federal government. Despite these challenges, MassHealth has developed proposals to improve payment efficiency while preserving services for MassHealth enrollees.
Starting immediately, MassHealth plans to conduct a competitive procurement that will focus on reducing costs while providing quality care to over 800,000 members. The procurement will include both the managed care and the Primary Care Clinician plan but will not include seniors or dual eligible members. The goals of the procurement are to ensure access and quality care for members at the lowest cost. MCO’s and providers who demonstrate the ability to provide this care will have the opportunity to expand membership. The procurement process will promote innovative approaches to care management and delivery as well as payments for services for this population. In addition, MassHealth will begin to lay the foundation for a comprehensive plan to promote the efficient delivery of care for MassHealth members under age 65 with a focus on care integration and care management for the highest-risk populations.
This procurement strategy will only mitigate a certain amount of growth in MassHealth costs that would otherwise occur. MassHealth plans to undertake several other steps such as constraining provider and capitation rates, limiting payments for preventable admissions, implementing small co-pays for some services, adopting additional program integrity measures, and limiting coverage for certain optional benefits.
Beginning in fiscal year 2011 and continuing in fiscal year 2012 and beyond, MassHealth will be launching a project to manage the dual population that is eligible for Medicare and Medicaid. A pivotal building block in systemic transformation to improve the delivery of health care and make health care costs sustainable for the long-term is MassHealth’s initiative to integrate Medicare and Medicaid for young dual eligible adults. MassHealth’s dual eligible adults ages 21-64 have disproportionately experienced the shortcomings of the fee-for-service payment system and fragmented, uncoordinated care, simply because few alternatives are available to them. MassHealth’s goal is to develop a Medicare and Medicaid integrated service delivery model option for dual eligible adults that:
- builds on Massachusetts’ knowledge and experience with integrated care programs;
- further promotes the goal of assuring that every member establishes a primary source of ongoing coordinated care;
- offers access to the benefits of integrated care, similar to what exists now for seniors;
- provides an alternative to the fee for service (FFS) system; and
- offers an option that meets individual needs and personal preferences.
MassHealth is engaged in discussions with consumer advisory groups to ensure that this new integrated care model meets the needs of the younger dual eligible population and is attractive to members so that they will want to enroll. The new model’s care entities will be accountable for the delivery, coordination, and management of health and community support services that promote improved outcomes and living with dignity and independence in the community. MassHealth envisions that the Medicare and Medicaid benefits would be administered jointly through an integrated financing mechanism at the state level such that dual eligible individuals would experience their coverage as a single, integrated care program. The Commonwealth is continuing to pursue this concept with the federal government.
| Fiscal Year 2012 MassHealth Cost Control Initiatives (in millions) | ||
| Gross | Net | |
| Rates | $ 150 | $ 75 |
|---|---|---|
| Capitation Cost Controls | $ 169 | $ 84 |
| Benefits/copays | $ 66 | $ 33 |
| Program Integrity | $ 13 | $ 7 |
| Procurement and Payment Strategies | $ 351 | $ 175 |
| Medicare Integration (Duals Initiative) | $ 50 | $ 25 |
| Total | $ 798 | $ 399 |
Commonwealth Care
The Commonwealth Care program was created with the enactment of health care reform and is administered by the Health Connector. The program provides health insurance coverage for individuals under 300% of the federal poverty level that do not have access to employer-sponsored insurance. Commonwealth Care fully subsidizes individuals under 100% of the federal poverty level and institutes a sliding scale of member premiums for those above that income threshold. It provides health care services through a fully capitated insurance model. As of January of 2011, there are 160,824 members enrolled in Commonwealth Care, excluding the Aliens with Special Status population (see next section on Commonwealth Care Bridge).
The budget provides $822 million for Commonwealth Care in fiscal year 2012, equivalent to currently projected fiscal year 2011 spending. These funds are designed to maintain eligibility for the program and pay for moderate additional enrollment (including coverage for individuals that transition from the Medical Security Plan to Commonwealth Care after their unemployment benefits expire).

The Administration envisions that the Health Connector will conduct a procurement process for the Commonwealth Care program, which will incent aggressive bidding and achieve savings by rewarding innovative, lower-priced health plans with increased membership. Under this vision, the Health Connector would strengthen existing program rules that currently provide incentives for some Commonwealth Care members to select lower-priced plans. This competitive procurement strategy would aim to leverage premium savings that enable the Health Connector to maintain eligibility for comprehensive coverage, pay for growing enrollment, and minimize increases in cost-sharing within a level-funded budget. In addition, the procurement will require MCO’s to work with the Health Connector in developing payment reform proposals in coordination with the MassHealth procurement. Overall, this approach intends to encourage game-changing innovations in contracting and care management that can help achieve sustainable health care cost savings inside and outside of the Health Connector.
Commonwealth Care Bridge
Aliens with Special Status (legal immigrants who have resided in the U.S. for less than five years) lost eligibility for Commonwealth Care in fiscal year 2010, due to the extreme fiscal challenges created by a national economic downturn and the fact that the federal government does not reimburse states for health insurance coverage for this population. Instead, a separate investment of $40 million was appropriated to provide health insurance for this population. This coverage is now available through the newly created Commonwealth Care Bridge program. The Commonwealth Care Bridge program was maintained in fiscal year 2011 at a projected cost of $50 million.
Commonwealth Care Bridge currently provides coverage to 20,389 Aliens with Special Status, who were enrolled over a three-month period from October to December of 2009. Enrollees have been eligible to receive comprehensive coverage through a network of providers that fully meets the Connector’s Commonwealth Care network adequacy standards. While cost-sharing is in some instances higher than that for Commonwealth Care and some benefits are excluded, steps have been taken to reduce any hardships for members.
The Administration’s fiscal year 2012 budget includes level funding of $50 million for the Commonwealth Care Bridge program. This program will continue to be run by the Secretary of Administration and Finance, the Secretary of Health and Human Services and the Executive Director of the Connector. The budget aims to maintain coverage for current Commonwealth Care Bridge enrollees through fiscal year 2012.
This funding for coverage for Aliens with Special Status reflects the Administration’s continuing commitment to providing health insurance to these legal residents of the Commonwealth. The Administration’s ultimate goal remains fully integrating Aliens with Special Status into Commonwealth Care. While that is not possible in the current fiscal environment (particularly given current federal reimbursement policy), national health reform will help by providing federal funding for subsidized coverage for Aliens with Special Status starting in 2014.
The Administration intends to keep the same benefit and cost-sharing structure for Commonwealth Care Bridge, given fiscal constraints and our goal of maximizing capacity of the program, but will continue to take steps to mitigate hardships.
Medical Security Program
The Medical Security Program (MSP) provides health insurance assistance for Massachusetts residents with family income less than 400% FPL, while they are receiving unemployment benefits. There are two different types of coverage offered through the MSP program: Premium Assistance and Direct Coverage. The Premium Assistance program is for COBRA eligible claimants, who may be reimbursed for up to 80% of their monthly premium, subject to a cap. The Direct Coverage program is for claimants not eligible for COBRA, or those who qualify for a waiver---they may enroll in coverage procured by the Division of Unemployment Assistance (DUA). There is no monthly premium for this option, but claimants are subject to equal co-payments at all income levels. The Medical Security Trust Fund which funds the Medical Security program has been under enormous fiscal stress due to continued extensions of unemployment benefits.
To pursue savings and improve alignment of state-subsidized health insurance programs, the Administration is requesting that the Health Connector work with the Division of Unemployment Assistance (DUA) to conduct a new, competitive procurement for MSP Direct Coverage and restructure the program to maintain eligibility for adults and children up to 400% FPL, while more closely matching Commonwealth Care coverage. Under this reform, members would receive coverage under plan types modeled after Commonwealth Care with a progressive cost-sharing and premium structure and improved continuity of coverage. The program would continue to be financed through employer contributions to the Medical Security Trust Fund. This initiative reflects a “shared responsibility” solution to maintaining health insurance coverage for families receiving unemployment assistance despite unprecedented fiscal stress on the Medical Security Trust Fund – combining recently increased employer contributions to the Medical Security Trust fund, program savings through a re-procurement and coverage re-design, and continued state contributions.
Group Insurance Commission
The Group Insurance Commission (GIC) will contain costs for state employees’ health care by negotiating lower rates and providing an incentive for employees to join limited network plans. The GIC will conduct a full open re-enrollment that will incent employees to move to limited network coverage, which costs less than broad network plans. The full open re-enrollment will require state employees to choose a plan during the annual open enrollment period in May. Historically, only 2% of active state employees actively select a plan during the annual open enrollment; those who do not are simply re-enrolled in their existing plan. In fiscal year 2012, state employees that move to a limited network plan will pay a lower premium for health insurance, as well as receive a reimbursement that is equal to three months of premium payments. The employees that move to the lower-cost plan in fiscal year 2012 will save on average an estimated $800 for individual coverage and $1,700 for family coverage. Employees moving to lower-cost plans will also result in tens of millions of dollars in savings for GIC. These savings, combined with controls on rate increases will allow the GIC to live with a level budget. Those employees who want to stay in a broad network plan will have that option.
.
Health Safety Net
Overseen by the Division of Health Care Finance and Policy, the Health Safety Net (HSN) reimburses hospitals and community health centers for health care services provided to low-income uninsured or underinsured residents. Prior to the enactment of health care reform, this financing mechanism was known as the Uncompensated Care Pool. The Health Safety Net is financed by dedicated revenues from an assessment on hospitals ($160 million) and an insurer surcharge ($160 million), other offsetting revenues ($70 million), and any state contribution from the General Fund.
Although success in expanding enrollment in health insurance through health care reform has resulted in decreased Health Safety Net utilization and payments, economic pressures from the recession have resulted in increased HSN utilization over the past three years. An unstable economy naturally lends itself to individuals ‘cycling’ in and out of short-term employment and underinsurance; the trends in the HSN from fiscal year 2010 through fiscal year 2011 reflect these natural increases in the burden on safety net care.
| FY10 | FY11 | FY12 | |
|---|---|---|---|
| Assesments | $320.00 | $320.00 | $320.00 |
| Offset | $70.00 | $70.00 | $70.00 |
| Commonwealth Contribution | $30.00 | $30.00 | $30.00 |
| Total Uses | $420.00 | $420.00 | $420.00 |
| FY10 | FY11 | FY12 | |
|---|---|---|---|
| Hospital Cost | $372.0 | $449-$474 | $449-499 |
| CHCs | $42.0 | $64.7 | $65.0 |
| DEMOS (Admin) | $6.0 | $6.0 | $6.0 |
| Total Uses | $420.0 | $420-$545 | $420-$570 |
To help reduce the burden on hospitals in Health Safety Net fiscal year 2011 (October 2010- September 2011) for providing care to the uninsured and underinsured, the budget provided $30 million in a General Fund contribution to offset 2011 costs.
Despite the unprecedented fiscal challenges of fiscal year 2012, the Administration is maintaining a $30 million General Fund contribution to the Health Safety Net in its fiscal year 2012 budget proposal. We will continue to closely monitor the Health Safety Net and refine projections for fiscal year 2011 and 2012 demand based upon updated information
Section III: Other Cost Containment Initiatives
Municipal Health Care
Municipal employee health costs are having a serious impact on local government finances and the provision of core municipal services such as education and public safety. Current municipal health insurance cost trends are not sustainable. The Administration is proposing a new local health insurance plan design process that will achieve material savings for cities and towns. This could save more than $94 million. In addition, all municipalities will be required to have their eligible retired local employees enrolled in Medicare as their primary source of health insurance coverage, as this federal program covers a substantial portion of their health costs. This is required of all eligible state employees and could save the 60% of municipalities not currently enrolled in Medicare $15 million to $30 million.
Small Business Health Care Cost Containment
The Health Connector will be launching updates in July to its Commonwealth Choice program, which creates a streamlined, simplified process for small businesses and individuals to shop for unsubsidized, name-brand health insurance, saving them money by making it easier for them to understand their options and choose better-priced health plans.
- The Health Connector will eliminate a fee it currently charges small businesses to shop through Commonwealth Choice. This fee was already significantly lower than those charged when small businesses shopped through other intermediaries, and now it will be eliminated starting in July.
- The Administration’s fiscal year 2012 budget includes $10 million (including $2.5 million contribution from the Health Connector) to enable the Health Connector to implement a provision of Chapter 288 calling on it to offer premium discounts for certain small businesses which purchase coverage through Commonwealth Choice and set up wellness programs for their employees. This will reduce premiums for qualifying small businesses by up to 5%.
- The Health Connector will be enhancing the Commonwealth Choice shopping experience by enabling small businesses and individuals to search whether a desired hospital or doctor is covered through the health plans they are considering.
Money Follows the Person Demonstration Project
In January 2011, Massachusetts applied to join Washington D.C. and the 29 other states already participating in “Money Follows the Person Rebalancing Demonstration” (MFP). With federal support, states will have additional programmatic and financial tools to rebalance their long-term care systems through the following:
- increasing the use of home and community-based services (HCBS);
- decreasing the use of institutional care;
- eliminating barriers that restrict flexible use of Medicaid funds; and
- ensuring quality assurance and quality improvement
The approval of the project will strengthen the Administration’s Community First initiative to transition long term care residents to the community from facility settings and improve MassHealth’s quality infrastructure, data resources and reporting capabilities. MassHealth also plans to create two new Home and Community-Based Waivers for MFP Demonstration participants who will need more intensive supports on an ongoing basis once they transition from facilities.
Patient-Centered Medical Home Initiative (PCMHI)
The Administration has committed to assist 46 primary care practices, including community health centers, hospital-affiliated primary care offices, and group and solo practices, to transition into certified medical homes focused on integrated and patient-centered care. PCMHI establishes a foundation for transforming the primary care landscape in Massachusetts through these pilot sites. It targets the elimination of fragmented and uncoordinated care delivery and improvements in chronic disease management. Patient-centered practices recognize the patient as an individual, respect the patient’s values, language and culture, and promote the exchange of information about care options between patients and providers.
Selected primary care practices will work toward mastering core competencies in patient-centered care over the course of three years and will receive training support, technical assistance and funding from the state. To help practices achieve core competencies and transform their operations, each participating practice will receive on-site, individualized coaching from a medical home facilitator and membership in a learning collaborative that includes in-person conferences, online trainings and evidence-based performance evaluation.
The Executive Office of Health and Human Services will oversee and evaluate the success and challenges of the pilot sites to further refine and spread the medical home model to additional practices in the future.
Electronic Health Record (EHR) Initiative
The American Recovery and Reinvestment Act of 2009 (Recovery Act) amended the Medicaid statute to provide for a 100% Federal financial participation (FFP) match for state expenditures for provider incentive payments to encourage Medicaid health care providers to adopt, implement, upgrade or meaningfully use certified EHR technology. It also established a 90% FFP match for reasonable state expenses related to administration of the incentive payments and to promote EHR adoption and health information exchange.
Adoption and meaningful use of interoperable EHRs can improve patient care in a number of ways including making the health care system more efficient by simplifying administrative procedures for doctors and patients; improving health care quality by making patient health information, available at all points of care; improving health outcomes and reducing costs through earlier diagnosis and characterization of disease; reducing adverse events through an improved knowledge of each patient’s medical history, potential for drug-drug interactions; and increasing efficiencies related to administrative tasks, allowing for more interaction with and secure transfer of information to patients, caregivers and clinical care coordinators.
The Administration is committing $500,000 as the state share to operate the implementation of the MassHealth Electronic Health Record (EHR) initiative, which will offer provider incentive payments with 100% federal participation funding to encourage Medicaid health care providers to adopt, implement, upgrade or meaningfully use certified EHR technology. MassHealth plans to distribute up to $50 million to approved health care entities to support transitions to electronic health record systems in fiscal year 2012.
[1] Kaiser Commission on Medicaid and Uninsured, “Hoping for Economic Recovery, Preparing for Health Reform: A Look at Medicaid Spending, Coverage and Policy Trends” September, 2010.
 top of page
top of page